Fungal nail infections (onychomycosis)
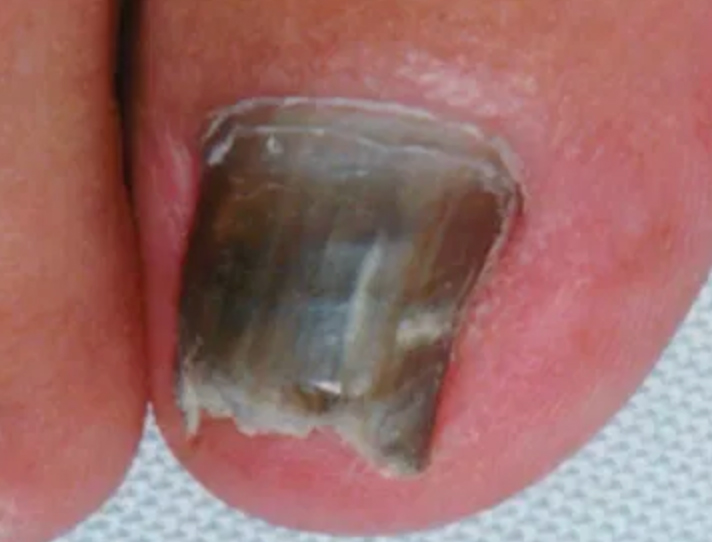
Fungal infection of nails is a common health problem which can be difficult to treat. The majority of sufferers don’t seek treatment, maybe don’t even recognise the existence of a problem. Surveys have shown that up to 30 % of people have onychomycosis with toenails more commonly affected than fingernails. Three groups of fungi cause this disease and these are known as dermatophytes (for example, Trichophyton rubrum), yeasts (for example, Candida albicans) and non-dermatophyte moulds (for example, Scopulariopsis brevicaulis); 85 – 90 % of fungal nail diseases are caused by the dermatophyte group of fungi. There is wide geographical and ethnic variation in the fungi that cause onychomycosis and an increase in foreign travel has lead to the introduction of some exotic species. In addition, fungi that were previously thought to be non-pathogenic may now occur as pathogens in patients with immune system deficiency, such as those with AIDS or leukaemia. Onychomycosis can be fatal in patients with a deficient immune system if the fungus infects tissue surrounding the nail and gains entry into the body.
Fungal nail infections look different depending on which fungi cause the infection however, when a fungal nail infection is suspected specimens should be taken to confirm the diagnosis and to identify the fungus involved. This is important because there are some dermatological conditions that look like onycomycosis, but in fact have a completely different cause and not all onycomycosis-causing fungi respond to all therapies.
Many localised nail infections caused by the dermatophyte fungi, non-dermatophyte fungi and Candidayeasts are treated with nail paints containing antifungal agents for example, tioconazole; these nail paints have a 40 % cure rate. If the surrounding tissue or nail bed is involved then the infection is very unlikely to respond to a nail paints. Terbinafine (Lamisil) is taken orally and is more effective than the nail paints. It will also treat infections where the surrounding tissue is affected and the cure rate for Terbinafine is 80-95 % for dermatopyte infections although it is less active against Candida yeasts and its activity against the non-dermatophyte moulds is unknown. Another group of drugs called the azoles can be taken orally for fungal nail infections. One of these drugs – itraconazole – has cure rate similar to terbinafine and is active against Candida yeasts, it is also active against some non-dermatophyte moulds. Griseofulvin can also be taken orally, but is only useful in dermatophyte infections, it has a cure rate of 90 % for fingernail infections, but only 40 % for toenail infections.
Some precautions can be taken to help prevent the development of fungal nail infections:
- Wash feet with soap and water and remember to dry thoroughly. Wear shower shoes in public areas and change socks daily.
- Nails should be clipped straight across so that the nail does not extend beyond the tip of the digit.
- Wear shoes that fit well and are made of materials that breathe.
- Avoid wearing excessively tight hosiery, which promotes the build up of moisture. Socks made of synthetic fiber tend to “wick” away moisture faster than cotton or wool socks, especially for those with more active life styles.
- The presence of an artificial nail or a polish impedes the evaporation of moisture from underneath the nail and the water trapped below can become stagnant and unhealthy, ideal for fungi and similar organisms to thrive.
- Always use preventive measures when applying polishes. Disinfect home pedicure tools and don’t apply polish to nails suspected of infection those on toes that are red, discolored, or swollen, for example.
Ringworm
Ringworm (tinea corporis) is a common infection usually acquired from other people, but also from animals. It is a worldwide problem. The usually appearance is non-symmetrical circular or oval patches with a slightly raised red edge and scaling. Usually the lesions are found on arms or legs but may be on the body or neck. Ringworm is not usually not itchy. The appearances may be quite different after application of local steroid ointment or other topical agents. If infections are from animals, they can be inflamed and pustular. There is a increasing problem with terbinafine resistance in some of the organisms causing ringworm.
Seborrheic dermatitis
Seborrhoeic dermatitis is found on the edge of the scalp, face and anterior chest and shows as red areas with scaling. It is caused by yeasts [Malassezia spp. or Pityrosporum spp.] that normally live on the skin but in some people leads to infection of the top (keratin) layer of the skin. Dandruff (or its equivalent in babies – cradle cap) is characterized by excessive scaling but minimal inflammation, and is largely a cosmetic problem.
Malassezia and eczema
Malassezia has been associated with two forms of eczema or dermatitis. The first, seborrhoeic dermatitis is an abnormal inflammatory reaction to Malassezia leading to a scaly rash on the face and scalp; dandruff is a mild form of this which is why it responds to antifungal containing shampoos. Malassezia can also provoke itchy facial eczema, called head and neck dermatitis, in young eczema-prone adults or atopics.
