The term mucormycosis (zygomycosis) is used to refer to infections caused by moulds belonging to the Order Mucorales. Common examples are bread moulds. These organisms can cause rhinocerebral, pulmonary, gastrointestinal, cutaneous or disseminated infection in predisposed individuals, the different clinical forms often being associated with particular underlying disorders. These infections are worldwide in distribution.
Mucormycosis is caused by moulds belonging to the Order Mucorales of the Class Zygomycetes. Many different organisms have been implicated, but the commonest causes of human infection are Rhizopus oryzae and R. microsporus. Other aetiological agents include Apophysomyces elegans, Cokeromyces recurvatus, Cunninghamella bertholletiae, Lichtheimia (formerly Absidia) corymbifera, Rhizomucor pusillus, Saksenaea vasiformis and Syncephalastrum racemosum.
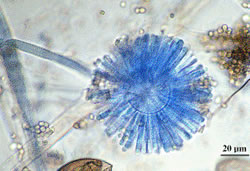
In tissue and in culture, these moulds form characteristic broad, non-septate or sparsely septate hyphae with right-angled branching. All these moulds cause similar diseases in humans, and the diagnostic and therapeutic approaches are similar. The species isolated from cases of human and animal infection are thermotolerant, and many are ubiquitous in the soil and on decomposing organic matter. These moulds are found in the indoor and outdoor air, on food items, and in dust.
Most human infections follow inhalation of spores that have been released into the air and the lungs and nasal sinuses are the commonest initial sites of infection. Infection may also follow cutaneous or percutaneous inoculation of organisms, either through traumatic disruption of skin barriers or as a result of cather insertion or injections. Less frequently, infection follows ingestion of contaminated food. Many of the aetiological agents of mucormycosis are ubiquitous in the environment and the likelihood that infection will occur following inhalation, implantation, or ingestion of spores largely depends on host factors.
The major risk factors predisposing individuals to the disease include prolonged or profound neutropenia, uncontrolled diabetic and metabolic acidosis, malnutrition, use of corticosteroids, and treatment with the iron chelating agent, desferrioxamine (deferoxamine). High risk patient groups include haematopoietic stem cell transplant (HSCT) recipients, solid organ transplant (SOT) recipients, patients with haematological malignancies, patients with type I or II diabetes mellitus, burns patients, injection drug users, and some individuals with no apparent immunological defects.
Certain predisposing conditions seem to be more commonly associated with particular clinical forms of disease. For instance, persons with diabetic ketoacidosis often develop fulminant rhinocerebral mucormycosis, while individuals with haematological malignancies and transplant recipients often develop pulmonary disease. Injection drug users frequently develop isolated cerebral infection. A significant number of cases of cutaneous mucormycosis occur in individuals with no underlying condition at the time of infection. In many of these cases, there is a history of penetrating trauma, burns, or road traffic accidents before the development of the infection.
In most countries, mucormycosis is rare, affecting about 1 in 500,000 annually. But in India, and other countries in the Indian sub-continent, the annual incidence is much higher – about 14 per 100,000. So about 211,000 are affected each year.
Amphotericin B used in high doses with resection surgery have been the mainstays of therapy for decades. Two new antifungals have now proven their worth for mucormycosis, usually given orally – posaconazole and isavuconazole.
